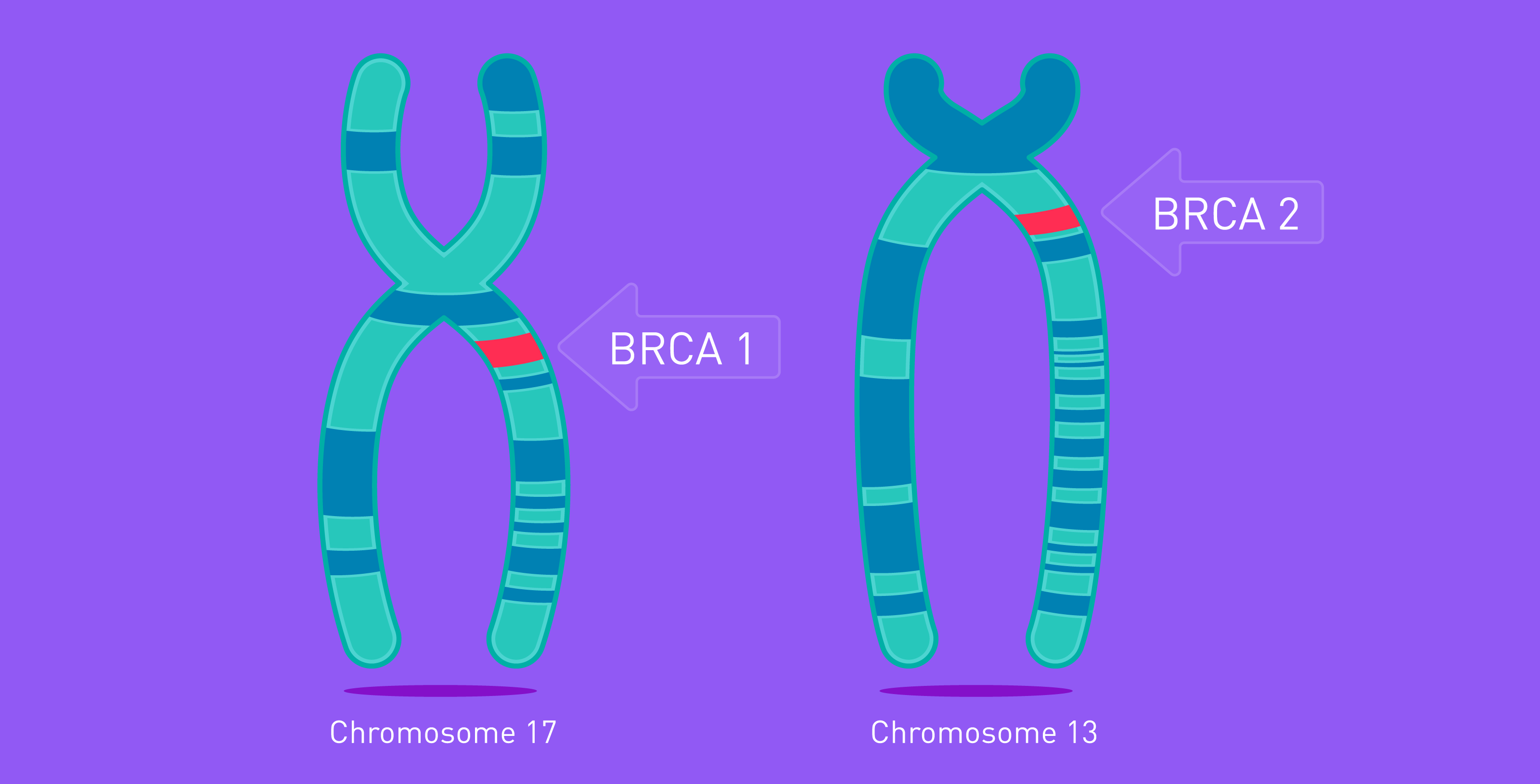
BRCA1 and BRCA2 are tumour suppressing genes. Find out what happens when you inherit mutated variants and how this impacts your risk of ovarian and breast cancer.
Table of contents
- What are BRCA1 and BRCA2 genes?
- How much do BRCA variants affect your risk of ovarian and breast cancer?
- Genetic testing for BRCA1 and BRCA2 variants
- Action steps if you test positive for a BRCA variant
- Takeaway
BRCA1 (BReast CAncer gene 1) and BRCA2 (BReast CAncer gene 2) are tumour suppressing genes that prevent cells from producing too quickly.
All humans have two pairs of these genes, one from their mother and one from their father. Some people inherit a mutated version of this gene, making them more susceptible to breast and ovarian cancer.
Faulty BRCA genes are the most common cause of hereditary breast cancer, accounting for about 5-10% of cases.
What are BRCA1 and BRCA2 genes?

BRCA1 and BRCA2 genes repair DNA damage that occurs during cell division. As such, they are known as tumour suppressing genes.
Everyone has a copy of BRCA1 and BRCA2, located on chromosomes 17 and 13, though some individuals inherit a mutated copy of the gene.
These harmful genes cannot repair damaged cells, sometimes resulting in tumours. To date, there are as many as 3000 variants of the BRCA gene known to cause disease.
About 1 in 400 people in the general population carry variants of these BRCA genes, though mutations are more common in certain ethnic groups.
In particular, those with Ashkenazi Jewish descent are more likely to carry variants in these genes with as many as 2% of Ashkenazi people testing positive. That works out at about 1 in 40 individuals.
Females with BRCA1 and BRCA2 gene variants have a significantly higher risk of developing multiple types of cancer, particularly ovarian and breast cancer.
They are also more likely to have cancer at a younger age and to develop cancer in both breasts.
Likewise, mutations in these genes increase a man's chance of developing prostate cancer, pancreatic cancer and, to a smaller extent, breast cancer.
Not everyone with these mutations will develop cancer, nor are they the only mutations associated with the disease; researchers have identified around 100 variants associated with cancer, though individually, many of these only increase someone's risk of developing cancer by a small degree.
How much do BRCA variants affect your risk of ovarian and breast cancer?
By contrast, 55%–72% of women who inherit a harmful BRCA1 variant will develop breast cancer by 80 years of age whilst 45%–69% of women with a BRCA2 variant develop cancer by the same age.
Both men and women with harmful BRCA1 and BRCE2 variants are at an increased risk of pancreatic cancer, though to a much smaller extent.
| Type of cancer | General population | BRCA1 | BRCA2 |
| Ovarian cancer | 1.2% | 39-44% | 11-17% |
| Breast cancer in women | 13% | 55-72% | 45-69% |
Risk of cancer by 70-80 years of age. Statistics sourced from the National Cancer Institute.
Genetic testing for BRCA1 and BRCA2 variants
There are a few reasons that a medical professional will refer you for genetic tests, including if you have a strong family history of cancer, a close relative has tested positive for a variant or if you experience breast cancer at a young age.
Before testing, individuals are sent for a risk assessment with a genetic counsellor.
These are trained professionals who can help you make informed decisions about genetic illnesses and decide on a course of action.
Genetic counsellors can refer patients for disease screening and help them access emotional support. Lastly, they can help you to interpret your results and respond accordingly.
Just because you do not have the BRCA gene variants, it doesn't mean that you can't develop breast cancer.
Many factors beyond genetics influence cancer risk, including diet, exercise levels, and smoking habits. Additionally, other variants besides BRCA1 and BRCA2 can influence cancer risk.
☝TIP☝ In 1980, two scientists interpreted a blue mark and swelling on Rembrandt's famous nude painting, Bathsheba At Her Bath, as an early sign of breast cancer. With the use of computer simulations, more recent research has concluded that it is "highly unlikely" the disease caused the blue mark or abnormality. However, the painting has become an icon for breast cancer nonetheless.
Action steps If you test positive for a BRCA variant
If you do test positive for harmful mutations in BRCA1 & 2 genes, there are proactive steps you can take to manage your cancer risk and improve your health prospects.
In particular, the chance of making a full recovery from breast cancer is relatively high compared to other forms, especially when detected and treated early.
Screening and self-examination
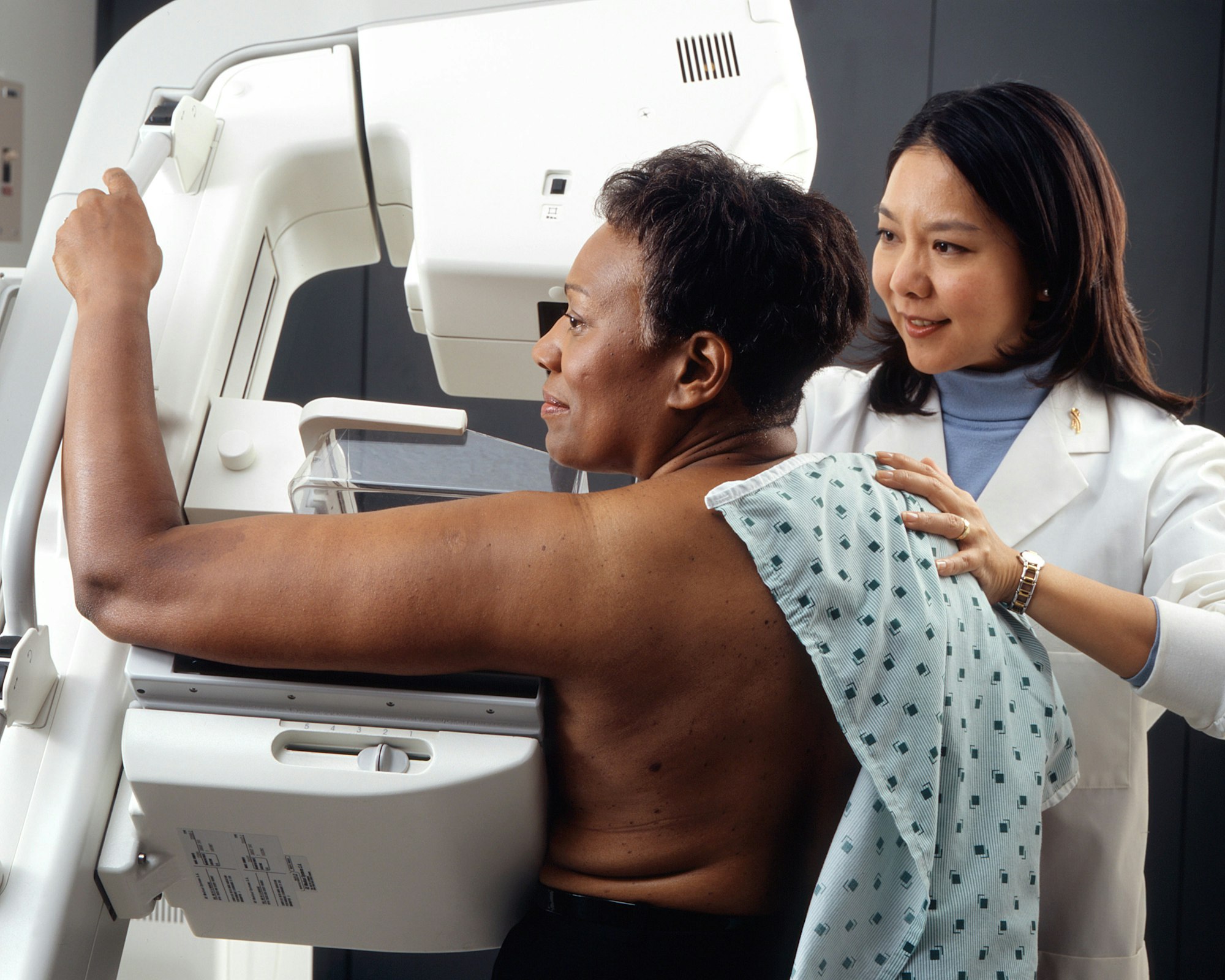
First and foremost, regular MRI screening and mammograms can help spot early breast cancer warning signs. If you carry a harmful variant, you should get screened more regularly than the average population.
Additionally, make a habit of examining your breasts and note any changes in the shape, size, feel or positioning. This applies to males with BRCA variants also as they are at an increased risk of breast cancer, albeit to a much smaller extent.
Symptoms of breast cancer include:
- Discharge from the nipple when not breastfeeding or pregnant
- Swelling or lumps under the armpits
- Change in size, shape or feel of your breast
- Rashes or dimpling on the breast
- Changes in the position of the nipple
There is currently no reliable screening method for ovarian cancer, though males with an altered BRCA2 variant can benefit from annual PSA blood tests for prostate cancer.
==☝Did You Know?☝ When you take the Atlas DNA Test, we screen for five different variants of the BRCA genes, including BRCA1 rs28897672, BRCA1 rs80357711, BRCA1 rs80357906, BRCA1 rs80357914, BRCA2 rs80359550. In total, there are 3700 variants currently known to cause disease. Speak to your GP if you are concerned a BRCA gene runs in the family.
Risk-reducing surgery
Women who carry a faulty gene can also get a mastectomy to reduce their cancer risk. During this procedure, tissue is removed from the breast to reduce the risk of cancerous growth's developing.
A preventative mastectomy reduces a women's cancer risk by as much as 50%, though it can be both emotionally and physically challenging. Those who undergo a mastectomy can opt to have silicon implants inserted in place of the removed tissue.
Additionally, women can undergo surgery to remove their ovaries and fallopian tubes, reducing their risk of developing ovarian cancer.
This procedure can also reduce premenopausal women's risk of breast cancer by removing a source of hormones known to fuel the growth of tumours. The removal of the ovaries triggers menopause in women and means they can no longer conceive a child.
Continuing, the risk of ovarian cancer in those with a faulty BRCA gene doesn't rise dramatically until after the age of 40, so some women choose to wait until then to have the procedure. A genetic counsellor can help you decide what course of action is best for you and your family.
Chemoprevention
Lastly, those with a harmful variant can also take preventative medication, namely tamoxifen and raloxifene. The Food & Drug Administration approves the use of these drugs in cancer prevention.
Nonetheless, there are potential side effects to using these drugs, and the National Institute For Health & Care Excellence (NICE) does not recommend taking them for longer than five years if you have no personal history of breast cancer. A genetic counsellor can discuss the merits and drawbacks of chemoprevention with you.
The Takeaway
- BRCA1 and BRCA2 are tumour suppressing genes that help repair DNA damage during cell division
- About 1 in 400 people inherit mutated versions of these genes.
- In women, mutated BRCA genes significantly increase the risk of developing cancer, particularly ovarian and breast cancer. In men, they increase the risk of developing prostate cancer, pancreatic cancer and breast cancer to a smaller extent.
- There are around 3000 disease-causing variants in BRCA genes.
- BRCA genes are more common in people with Ashkenazi Jewish heritage.
- If you have a strong family history of cancer, a relative who has tested positive for a variant or if you experience breast cancer at a young age, you are likely eligible for a genetic test.
- Those who test positive can take measures to minimise their risk, including frequent screening, self-examinations, preventative surgery, and chemoprevention.
☝️DISCLAIMER☝This article is for informational purposes only. It is not intended to constitute or be a substitute for professional medical advice, diagnosis, or treatment.