In honour of May Measurement Month, we are taking a look at the DASH diet, an eating plan proven to lower blood pressure and protect against cardiovascular disease.
High blood pressure is the leading cause of preventable death each year, claiming ten million lives annually. Despite this, only half of those affected know they have the condition.
Launched in 2017, May Measurement Month is a global blood pressure screening campaign offering free BP checks to those 18+.
To register interest in blood pressure screening, visit the May Measurement Month website. If you can’t attend a screening centre, worry not- validated blood pressure monitors are inexpensive and straightforward to use.
Table of contents
- What is hypertension?
- Understanding your blood pressure reading
- The DASH Diet to lower blood pressure
- The DASH eating plan
- Will the real DASH please stand up?
- Top tips when transitioning to DASH
What is hypertension?
In the UK, it is estimated that one-third of individuals may be suffering from hypertension
Over time, high blood pressure can diminish the elasticity of the arteries and cause scarring, leading to heart disease, stroke, congestive heart failure, kidney disease, and even blindness if left untreated.
High blood pressure is commonly associated with poor lifestyle habits, such as smoking, a sedentary lifestyle, excessive drinking and an imbalanced diet. Even being slightly above the ideal level for extended periods can increase your risk of health complications.
The good news is that once it has been diagnosed, the condition can be successfully treated with medication as well as lifestyle and dietary changes.
The only way to know if you have high blood pressure is to get a blood pressure test, which can be performed in surgery or at home.
☝TOP TIP:☝ If you are taking a blood pressure measurement at home, it is important that you do not smoke or drink coffee/alcohol for 15 minutes prior to the test.
Understanding your blood pressure reading
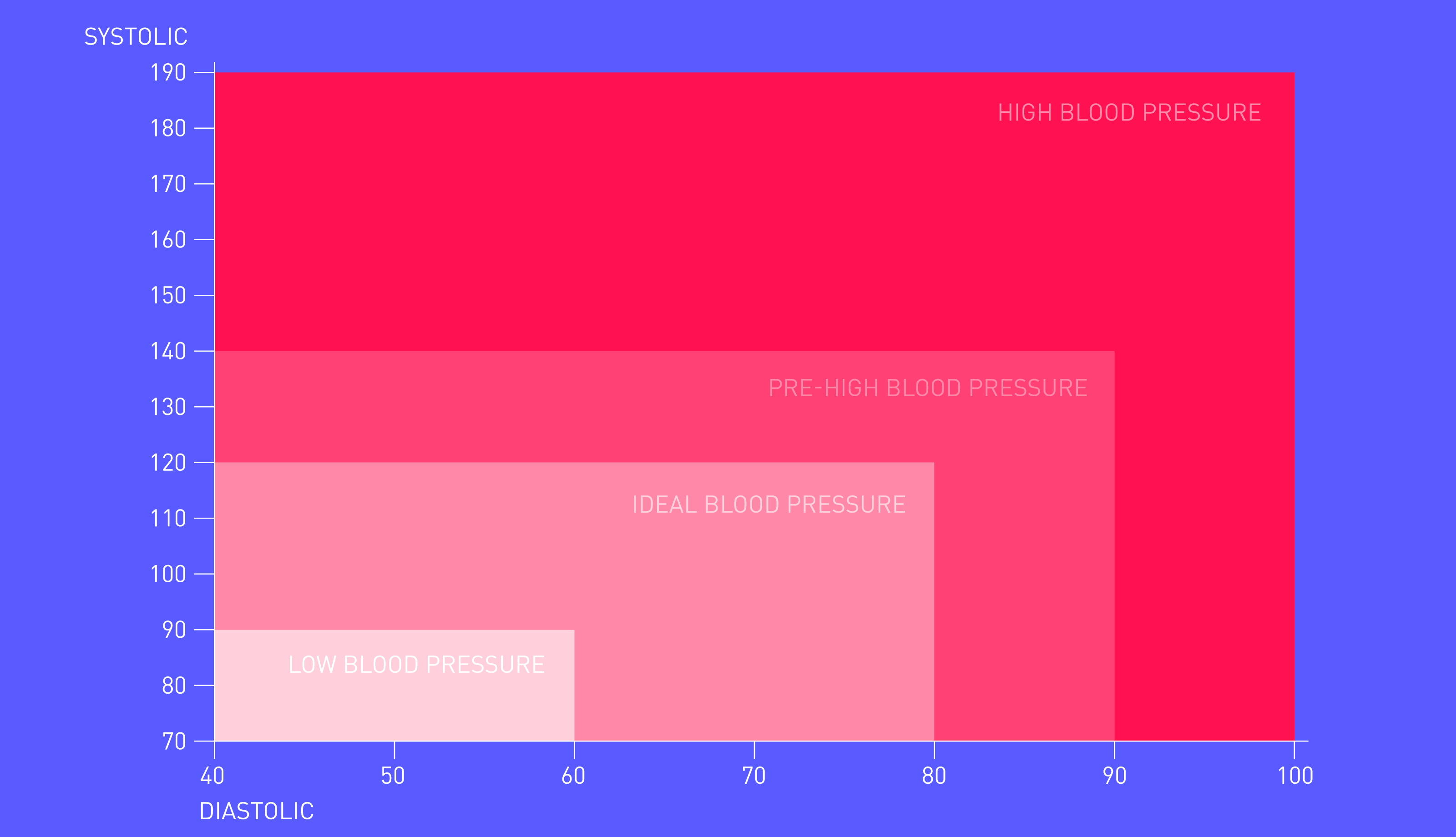
A blood pressure reading consists of two numbers: the systolic and diastolic reading.
Systolic is the first number in a BP reading and indicates the pressure in the arteries when the heart beats; diastolic is the second number and indicates the pressure in the arteries between beats.
For example, if the first number is 120 and the second number is 80, this would be written as 120/80, or 120 over 80.
Blood pressure is measured in millimetres of mercury (mmHg) so the reading would be 120/80mmHg, which is at the upper end of the ideal range.
Below, we’ve listed what qualifies as high, ideal, and low blood pressure. If you measure your BP at home, you can check your results on both the NHS and May Measurement Month websites.
As a general guide:
High blood pressure: 140/90mmHg or higher (or 150/90mmHg or higher if you're over the age of 80).
Pre-high blood pressure: 120/80mmHg to 140/90mmHg
Ideal blood pressure: Between 90/60mmHg and 120/80mmHg
Low blood pressure: Under 90/60mmHg
If your blood pressure consistently reads as between 130-139/80-89mmHg, this is known as hypertension stage 1. At this point, your doctor will recommend lifestyle changes and potentially medication, depending on your risk of heart-related disease.
The more your blood pressure rises above normal, the greater the health risk
Your doctor will most likely prescribe blood pressure medicine and lifestyle changes if your blood pressure consistently ranges at 140/90mmHg or higher. BP readings in this ballpark are known as hypertension stage 2.
Lastly, a blood pressure reading of 180/120mmHg or higher is known as a hypertensive crisis and requires immediate medical attention.
If your blood pressure isn't too high, you may be able to control it entirely by making lifestyle and dietary changes, such as losing weight, managing stress, quitting smoking, and following the DASH diet.
The DASH diet to lower blood pressure
Diet is an important line of defence against high blood pressure, with the gold standard of diets used to treat the condition being DASH, standing for Dietary Approaches to Stopping Hypertension.
The DASH Diet enjoys endorsements from the National Heart, Lung and Blood Institute (NHLBI), The Kidney Foundation, and The American Heart Foundation.
Although referred to as a diet, this is misleading; DASH is a flexible eating plan that requires no special foods, instead offering general food principles based on heart-healthy guidelines.
Additionally, the eating plan suggests reducing your intake of tropical oils such as coconut or palm.
DASH was first formulated in 1996 by The American Heart Foundation, mainly by two figures: Dr Frank Sacks, Professor of Medicine at Harvard Medical School, along with Dr Lawrence Appel, Professor of Medicine at Johns Hopkins University.
Shortly afterwards, they published a landmark clinal study in the New England Journal Of Medicine demonstrating its efficacy in reducing blood pressure.
Known as the DASH trial, the study randomly assigned 459 participants to one of three diets; a control diet which mimicked the standard American diet; the same diet but with more fruit and vegetables and the DASH diet, which is rich in vegetables, fruit and low-fat dairy foods whilst lower in saturated fat, total fat and cholesterol.
All the diets contained around the same amount of sodium, roughly 3000 mg daily- less than the average American eats but higher than the recommended amount.
Both the fruit/vegetable diet and the DASH diet reduced blood pressure, though the effects of the DASH diet were more pronounced. The DASH diet reduced systolic and diastolic blood pressure by 5.5 and 3.0 mmHg more than the control diet.
In contrast, the fruits-and-vegetables diet reduced systolic blood pressure by 2.8 mm Hg and diastolic blood pressure by 1.1 mm Hg more than the control.
Besides lowering blood pressure, the DASH diet also lowered low-density lipoprotein (LDL) levels, colloquially known as bad cholesterol.
The reduction of blood pressure in the DASH combination diet was comparable to that of people on medication for stage 1 hypertension, particularly impressive considering it was independent of sodium reduction.
A second DASH trial, comprising 412 participants, compared the effects of a reduced-sodium intake on both the DASH and standard American diet.
In short, participants were assigned to one of the two eating plans and then followed for a month whilst consuming either 3300mg, 2300mg or 1500mg of salt daily.
Reduced sodium intake lowered blood pressure in both groups but was more significant in those following a DASH diet.
As expected, 1500mg of salt daily on a DASH diet plan produced the greatest reduction in blood pressure. Whilst the first DASH trial capped sodium intake at around 3000mg daily, the official DASH eating plan now caps this at 2300mg.
Besides improving blood pressure and protecting against heart disease, the diet is rich in plant-based fibre and prebiotics, meaning foods which nourish beneficial bacteria in the gut. As such, a DASH eating plan can boost microbiome diversity and potentially encourage probiotics.
What’s more, the diet has also been shown to reduce uric acid levels in those with hyperuricemia (excess uric acid), meaning it can potentially protect against the inflammatory disease gout.
Last but not least, adherence to a DASH diet may also be able to prevent the development of type 2 diabetes also.
The DASH eating plan
The DASH diet encourages you to increase your intake of vegetables, fruits, whole grains, legumes, nuts, fish, poultry and healthy vegetable oils. Simultaneously, the diet recommends limiting your consumption of red or fatty meats, sugar-sweetened drinks, sweet treats, full-fat dairy and salt.
The number of suggested servings of each food group is dependent on your calorific needs. The NHLBI has a chart to help you calculate this, factoring in your age, gender and activity levels.
Besides the amount of servings required in each food group, the specifics are left for you to decide, allowing for flexibility. The following diet is an example of the recommendations and serving sizes for those requiring 2000 calories daily:
| Food Group | Daily Servings |
| Grains | 6-8 |
| Meats poultry and fish | 6 or less |
| Vegetables | 4-5 |
| Fruit | 4-5 |
| Low-fat or fat-free dairy products | 2-3 |
| Fats and oils | 2-3 |
| Sodium | 2300mg |
Additionally, the recommendations for those on a 2000 calorie diet suggest 4-5 servings of nuts, dry beans, seeds and peas a week, and no more than five servings of sweets weekly.
Whilst the table recommends 2300mg of sodium, reducing this to 1500mg can lower blood pressure even more drastically.
Will the real DASH please stand up?

If you hear people refer to the “original” DASH diet, they mean the one followed in the 1997 trial. Since then, numerous modified DASH diets have emerged, namely the Omniheart DASH diet and a Mediterranean DASH diet.
In short, these versions of the DASH diet substitute some of the recommended carbohydrates in the original for either healthy fats or proteins.
Instead, the Mediterranean DASH diet makes up these calories with an extra 8% of monounsaturated fats and 2% of polyunsaturated ones. These can be found in oily fish such as salmon and nuts.
The Omniheart DASH makes up for these with an additional 10% of protein derived calories, mainly from nuts, seeds, legumes and grains.
In a 2005 randomised clinical trial, both of these modified DASH diets were shown to reduce blood pressure levels and heart disease risk more significantly than the original DASH diet.
Compared with the original DASH diet, the Omniheart diet decreased mean systolic blood pressure by 1.4 mmHg and 3.5 mmHg among those with hypertension.
Likewise, the Mediterranean DASH diet enriched in unsaturated fats decreased systolic blood pressure by 1.3 mm Hg and diastolic blood pressure by 2.9 mm Hg compared with the original DASH.
Top tips when transitioning to a DASH diet
Based on the recommendations suggested by the NHLBI, we have compiled a list of top tips to help you transition to a DASH Diet.
- Instead of loading up on red or fatty meats, substitute meat and poultry for fish twice a week
- Opt for meatless meals once or twice a week. For example, switch out mincemeat for vegetables in your bolognese or trade chicken wings for cauliflower wings
- When you eat meat, pick lean cuts and remove the skin from poultry
- Opt for beans or seeds instead of nuts if you have an allergy
- Steer clear of refined grains and choose whole grains instead, as these contain more nutrients, minerals and fibre
- If you are not used to eating lots of fibre, introduce this gradually to avoid digestive upset
- Snack on fruits, vegetables and nuts in favour of crisps and sweets
- Keep a bowl of fruit near your desk
- Use herbs and spices instead of salt to add flavour to meals (garlic and lemon juice). Bonus: garlic and ginger are prebiotic!
- Incorporate your recommended foods from the Atlas Health dashboard into the DASH eating plan
- Aim for a variety of fruits and vegetables

==☝️DISCLAIMER☝This article is for informational purposes only. It is not intended to constitute or be a substitute for professional medical



















