In honour of Breast Cancer Awareness Month, we weigh the pros and cons of hormonal contraceptives so you can make an informed decision based on facts, not fear.
- Breast Cancer Awareness Month
- What are hormonal contraceptives, and how do they work?
- The link between hormonal contraceptives and breast cancer risk
- How much do hormonal contraceptives increase your breast cancer risk?
- Who shouldn't take oral contraceptives?
- The benefits of oral contraceptives
- Final thoughts
- Article summary
Breast Cancer Awareness Month

October marks Breast Cancer Awareness Month, an annual campaign to encourage screening for, and educate the public on, breast cancer.
In the UK, around 1 in 8 women develop breast cancer in their lifetime, but not everyone's risk is the same; lifestyle, genetics, age and certain medications can all influence your unique risk for the disease.
Although hormonal contraceptives are linked to a slight increase in breast and cervical cancer risk, multiple studies show that hormonal contraceptives can reduce your risk of other types, namely ovarian, uterine and colorectal cancer.
Accounting for these protective effects, they may reduce your total risk of cancer.
Those with a history of breast cancer are strongly advised against hormonal contraceptives, which can increase the risk of relapse.
Moreover, if you're at an increased risk for breast cancer already- because of harmful genetic mutations, for example- it may be wise to avoid hormonal contraceptives.
To assist you in making a decision, we've broken down the research looking at hormonal contraceptives and cancer risk. Let's jump in:
What are hormonal contraceptives, and how do they work?

Oral contraceptives- often referred to as "the pill"- are a popular form of hormonal birth control.
The most common oral contraceptive type is the "combined contraceptive", which contains synthetic versions of oestrogen and progesterone- naturally occurring female sex hormones.
The progesterone-only pill- also called "mini-pill" or POP- is another form of oral contraceptive that only contains the hormone progesterone.
The link between hormonal contraceptives and breast cancer risk
Observational studies show that the combined contraceptive pill is linked to a small increased risk for breast and cervical cancer.
However, they are also associated with risk reductions for colorectal, ovarian and uterine cancers.
Naturally occurring oestrogen and progesterone can fuel the growth of specific cancer cells, so it's suspected that the synthetic versions in combined contraceptives are responsible for increased breast cancer risk.
Newer generations of the combined pill contain less of these hormones than those designed 30 years ago, although they are still linked to a slight increase in risk.
It's unclear whether the "mini-pill" increases cancer risk, and if so, by how much. Some studies suggest it's linked to cervical and breast cancer, although the evidence is inconclusive.
How much do hormonal contraceptives increase your breast cancer risk?

The primary studies looking at oral contraceptives and breast cancer risk are observational studies, three of which we shall briefly explore.
The first is a meta-analysis of around 54 epidemiological studies comprising 150,000 women.
Moreover, those who were actively using oral contraceptives were shown to have a 24% increase in risk.
Risk levels declined when women stopped taking the pill, returning to normal after about ten years.
It's important to note that these are relative risks, which say nothing about a woman's absolute or actual risk for breast cancer.
To know how much contraceptives increase breast cancer risk, you need to know a woman's baseline risk without taking contraceptives.
Breast cancer is rare in young women, so the increased risk of developing breast cancer is extremely small up to around 39 years old.
Experts generally agree that women below 50 without a family history of breast cancer or harmful genetic mutations have an absolute risk of around 2%.
In women fitting this profile, a 24% increase refers to 2%, meaning contraceptives raise this by about 0.50%.
The second study analysed 116,000 women between 24-43 years of age, all of which were enrolled in the Nurses Health study- one of the largest and longest-running prospective studies to date.
In line with previous studies, they found a slight increase in breast cancer risk for those actively using hormonal contraceptives (33%) but not for those who had taken them historically.
A large majority of the increased risk was attributed to a specific type of contraceptive called the "triphasic" pill, which changes the dose of hormones every seven days throughout a woman's period.
The researchers observed a particularly significant increase in risk for women using triphasic contraceptives with levonorgestrel as the progestin; women taking these pills were 3.5 times more likely to develop breast cancer than those who had never taken a contraceptive.
The third study is more recent, appearing in the New England Journal Of Medicine in 2017.
The prospective cohort study sought to quantify how much newer forms of oral contraceptives influence breast cancer risk.
Using national medical records, the researchers tracked 1,797,932 Danish women for around 11 years to determine how hormonal contraceptives influenced health outcomes.
Overall, women who were using or had recently stopped using oral combined hormone contraceptives had a modest (about 20%) increase in the relative risk of breast cancer compared with women who had never used oral contraceptives.
Put more simply, the increase in risk was about one new breast cancer case per 7,690 women who used hormonal contraceptives for a year.
In women under 35, the increase was even lower, equating to about one additional breast cancer case for every 50,000 women who used hormonal contraceptives for a year.
The study found that a levonorgestrel-releasing intrauterine device increased breast cancer risk by about 21% also.
As for progesterone-only pills, some showed no increased risk, whilst others (oral levonorgestrel in particular) were linked to increases of up to 21%..
According to Breakthrough breast cancer, for every 2000 women up to the age of 59 not using combined contraceptives, 90 are expected to have breast cancer.
In 2000 women using the combined pill, 112 can be expected to develop the condition.
Your risk will depend on multiple factors, such as your lifestyle, diet and genetics.
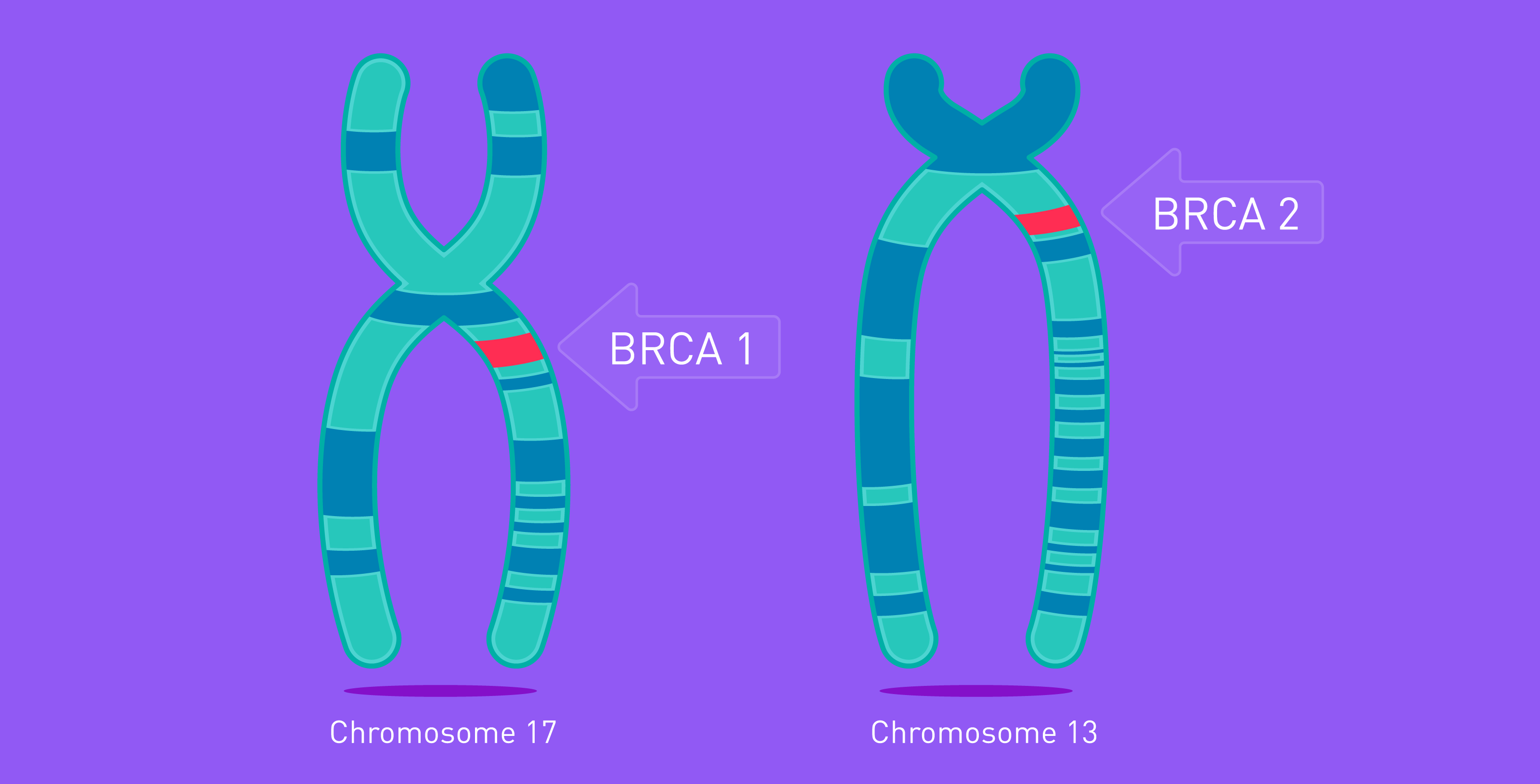
For example, BRCA 1 and 2 gene mutations, smoking cigarettes, excessive alcohol, and obesity are also associated with increased risks for breast cancer.
Who shouldn't take oral contraceptives?

If you've been diagnosed with breast cancer in the past, it is recommended that you do not take hormonal contraceptives such as the combined pill.
Additionally, those with harmful BRCA genes or a family history of breast cancer should consult their doctor or family planning clinic before starting hormonal birth control pills.
If your breast cancer risk is higher than average, there are non-hormonal birth-control alternatives available to you, including
- Condoms
- diaphragms
- non-hormonal intrauterine devices (IUDs)
- Permanent surgical birth control
Oral contraceptives are linked to an increased risk for cervical cancer, so women at high risk for the condition may also wish to avoid them.
One study found that oral contraceptives increased cervical cancer risk by 10% when used for less than five years, 60% for 5–9 years and 50% after ten or more years of use.
The benefits of oral contraceptives
It is vital that we interpret the risks of oral contraceptives in light of their benefits.
Besides being a highly effective form of birth control- boasting 91% success rates- they have been shown to slightly reduce a person's risk for ovarian, colorectal and uterine cancer.
For example, women taking combined contraceptives are 30-50% less likely to develop ovarian cancer relative to women who have never used them.
For reference, a women's absolute lifetime risk of being diagnosed with ovarian cancer is about 1 in 50 (2%).
In other words, taking the hgihest number (50%) would mean oral contraceptives reduce ovarian cancer risk to 1%.
Oral contraceptives are also associated with a 15-20% reduction in colorectal cancer risk and around a 30% reduction in endometrial cancer risk also. Bear in mind these are relative risk reductions.
According to some studies, oral contraceptives may reduce your total risk for cancer when these benefits are registered.
It's not entirely clear how hormonal contraceptives reduce a person's risk of bowel, uterine and ovarian cancer, though researchers have a few ideas, including:
- They reduce bile acids in the blood (colorectal cancer)
- They lower exposure to oestrogen and progesterone by preventing ovulation (ovarian cancer)
- They prevent cancerous cell growth in uterine tissue (endometrial cancer)
Final thoughts
Epidemiological studies show that hormonal contraceptives, particularly the combined pill, can slightly increase a woman's risk of breast cancer.
However, the combined pill is also associated with a reduced risk for colorectal, ovarian and uterine cancer.
In women under 50 with no genetic predispositions, the risk for breast cancer is low- as is the relative increase when taking hormonal contraceptives.
More specifically, the pill causes about 14 extra cases of breast cancer in every 10,000 women between 30-39 taking the pill.
A woman's risk for breast cancer increases as she ages- which hormonal contraceptives slightly inflate.
For most women (especially those under 40), the benefits of the combined contraceptive will outweigh the risks, but the significance of the increased risk is unique to every woman.
Those previously diagnosed with breast cancer should not take hormonal contraceptives.
Moreover, anyone at an increased risk for breast cancer should consult their GP or a family planning clinic before starting hormonal contraceptives.
Article summary
- Studies show that the combined contraceptive pill can slightly increase your breast and cervical cancer risk, likely because they contain oestrogen and progesterone.
- The increased risk for breast cancer is relatively small, especially in women under 40 without a history of breast cancer in the family.
- A women's risk for breast cancer increases as she ages, especially in those over 50.
- If you are at an increased risk for breast cancer, you should consult your doctor or family planning clinic before starting hormonal contraceptives.
- If you have previously been diagnosed with breast cancer, you should not take hormonal contraceptives.
- The risks of taking the combined contraceptive pill must be interpreted in light of its benefits, namely a reduced risk for ovarian, uterine and colorectal cancer.
- For most women, the benefits of taking combined contraceptive pills will outweigh the risks. However, the importance of the increased risk varies between women.
☝️DISCLAIMER☝This article is for informational purposes only. It is not intended to constitute or be a substitute for professional medical advice, diagnosis, or treatment.