Obesity isn’t just another name for excess weight. Learn what causes the disease, the associated risks, and how genes are involved.
Obesity is a chronic disease characterised by excessive fat deposits in the body. The condition is a growing public health issue and affects more than 2 billion people globally. According to the NHS, more than 24% of British citizens are obese, whilst another 60% are overweight.
Table of contents
- Obesity and metabolic syndrome
- Identifying obesity
- What causes obesity?
- The role of genetics in obesity
- Tackling obesity: treatment methods
- Key takeaways
Obesity and metabolic syndrome
Obesity can increase a person’s risk of developing numerous severe conditions. A large majority of these conditions arise via metabolic syndrome, a condition that is co-morbid with obesity.
Metabolic syndrome is a cluster of conditions that occur together, putting a person at high risk of developing cardiovascular diseases, cardiac arrest, pre-diabetes, and diabetes type II.
Conditions that make up metabolic syndrome include:
- High blood pressure
- High blood sugar
- Excess body fat around the waist
- Abnormal cholesterol levels
Besides metabolic syndrome, obesity can also cause sleep apnea, a condition where your breathing stops periodically whilst at rest.
Sleep apnea can lead to oxygen desaturation, thereby increasing your risk of heart failure, cardiovascular disease and hypertension (high blood pressure).
Furthermore, obesity has been linked with joint issues due to increased weight and can raise your risk of developing 13 types of cancer.
Lastly, obesity adversely affects the endocrine system because adipose fat tissue in the abdominal area is involved in sex hormone regulation. In obese women, excessive hormone precursors transform into oestrogens, leading to a hormonal disbalance.
In the UK, obesity is the second biggest cause of cancer behind smoking, totalling about 18,100 cases annually.
As a result, obese women may face problems during conception and experience complications throughout pregnancy.
How to identify obesity
So when does excess body weight transition to obesity? One way to measure this is by calculating your BMI, which can be found by dividing your body mass (kg) by height in square metres.
Reference example
Weight: 60 kg
Height: 1.7 m.
60 / (1.70 * 1.70) = 20.7
BMI = 20.7 kg/м2.
☝IMPORTANT☝ This is a very simplified formula. The NHS has a special online BMI calculator that accounts for several important criteria beyond weight and height, such as sex, age, and physical activity levels.
Your BMI results are then compared with the reference numbers below to determine obesity risk:
| 18.5–24.9 | Norm |
|---|---|
| 25–29.9 | Excessive weight |
| 30–39.9 | Obesity |
| Over 40 | Extreme obesity |
With that said, a high BMI can be a warning sign of obesity, especially when used in conjunction with other methods, as we will explore now.
Waist circumference
A waist circumference test can help to estimate your potential risk for obesity. Whilst the test can be used as a screening tool, it is not diagnostic of either your health or the amount of fat present.
To perform the test, place a measuring tape just above the crest of the pelvic bone and wrap it around the waist. Next, inhale and exhale calmly without effort, and record the results.
A male waist circumference of 40 inches or more may indicate an increased risk for obesity.
In non-pregnant women, a waist circumference of 35 inches may suggest an increased risk also, though the results should be interpreted by a trained healthcare professional.
A waist measurement test is better for people who carry a lot of muscle and less fat, like bodybuilders, boxers and other athletes.
Waist to hip ratio
To measure the circumference of the hips, put your feet together, place the tape on the most protruding point of the thigh and wrap it around. Lastly, divide the waist circumference by the hip circumference.
A waste to hip ratio of more than 0.9 for males and 0.85 for females could indicate an increased risk for lifestyle diseases.
☝IMPORTANT☝: Waist to hip measurement is not recommended for children.
Skinfold thickness
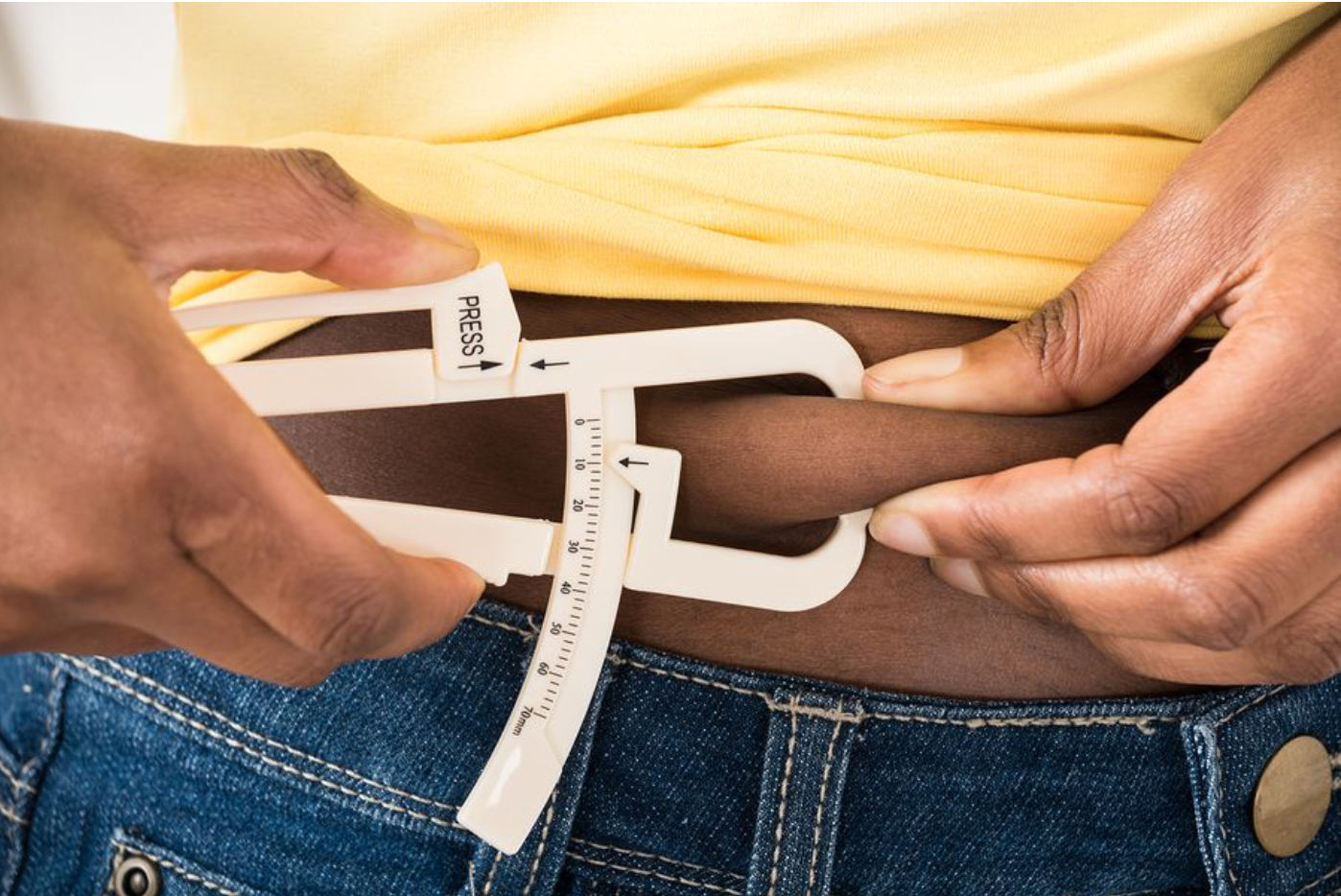
To measure skinfold thickness, you need a special tool called a calliper.
A doctor will pinch a skin fold in the abdominal area, hips, and the upper part of your back. Based on skinfold thickness, they will calculate your body fat content using a special formula.
Bioimpedance method
Bioimpedance involves special devices that pass a safe multi-frequency pulse through the body.
Doing so can determine the level of tissue electrical resistance, allowing you to calculate the percentage of fat and muscle in the body.
Bioimpedance analysers are available in many clinics, nutritionists' offices and even some gyms. You can also purchase scales with this technology built-in for home use.
The method is relatively accurate, though errors can occur if the measurement is taken during illness or after vigorous physical activity. In both cases, results are skewed due to a change in the ratio of water and fat.
What causes obesity
Many assume obesity is solely due to poor diet and sedentary lifestyles. Sadly, stigma surrounds the condition, with people assuming that obesity results from laziness and lack of willpower.
In reality, the condition is a multifactorial disease with complex and varied causes. Besides how and what someone eats, there are a confluence of factors that can lead to obesity, including genetics, sleeping pattern and mood disorders.
Moreover, excessive fat can be the consequence of other health conditions as well, including
- Hypothyroidism (thyroid hormones deficit)
- Cushing syndrome (excess adrenal hormones)
- Polycystic ovarian syndrome (impaired ovarian function)
Continuing, certain medications such as hormonal medications (corticosteroids), sugar-lowering agents in the blood, antidepressants, antiepileptics, and some drugs for chemotherapy can also cause rapid weight gain.
The role of genetics in development of obesity
Up to 70% of obesity cases are associated with genetic mutations. More than 50 genes are known to affect the development of the disease.
For example, obesity may be associated with a deficiency of melanocortin receptors triggered due to abnormalities in the MC4R gene.
The MC4R gene regulates eating behaviour and appetite suppression, so it’s not hard to see how it could affect body weight.
Up to 6% of people who have suffered severe obesity since childhood have mutations in the MC4R gene.
Melanocortin is a hormone that is responsible for feeling full. As such, If the functioning of the MC4R gene is disrupted, a person may be predisposed to overeating.
Mutations in the FTO (fat mass and obesity-associated) gene may also be responsible for the development of obesity.
The good news is that DNA is not your destiny; numerous studies show that those with a genetic predisposition to obesity can successfully manage weight.
Moreover, whilst genetic factors are one of many pathways to obesity, they are not the sole, or even the primary, cause. Instead, obesity is a multifactorial disease that results from a patchwork of factors- both genetic and environmental.
Tackling obesity: treatment methods
There are numerous treatment options for obesity, ranging from lifestyle and dietary changes to psychiatric or surgical interventions.
When choosing a treatment plan, always consult a specialist. Drawing on their experience, they can decide which options best suits your unique circumstances.
For example, weight gain triggered by an underlying health condition like hyperthyroidism requires different treatment than someone overeating due to a mood disorder.
Without further ado, let’s explore a few ways you can prevent and tackle obesity.
Change your diet

A nutritionally balanced and calorie-controlled diet is an effective intervention for obesity. Steer clear of fad diets or restrictive eating plans and aim to improve your nutritional intake gradually.
Losing anywhere between 0.1–and 1kg per week is considered healthy. Better still, gradual weight loss is associated with a reduced risk of regaining weight down the line!
Start by adding healthy foods to your diet, e.g., veggies and greens to every meal, and substitute unhealthy options for more nutritious alternatives. For example, you could swap out ice cream with yoghourt and seasonal fruits!
It is impossible to control the ingredients used and the amounts in the dishes you order when you eat out.
With this in mind, limit takeaways to the weekend and make an effort to cook at home throughout the week. That way, you can control how much salt, sugar, and other ingredients you consume.
Below are some simple dietary changes you can make to tackle obesity:
- Add more vegetables and fruit to your diet
- Eat foods rich in protein
- Choose healthy sources of fats
- Cut down on processed foods
- Avoid sugary drinks
According to Canada’s Official Food Guide, the “ideal plate” should be balanced as follows:
½ — fruit and vegetables
¼ — protein-rich foods
¼ — cereals and wholegrain foods
As well as focussing on what you eat, it is equally important to pay attention to how, when and why you eat also.
In some cases, overeating may result from boredom, whilst others may eat so quickly they don’t allow themselves time to feel full.
By being mindful of your eating habits, you can discover meaningful insights and make necessary changes.
Lastly, studies suggest that personalised dietary recommendations are more effective than generalised nutritional advice at reducing fat, sugars and salt in the diet.
Move more

Physical activity aids with weight loss and has an overall beneficial effect on health and mood. In general, you should aim for around 30-40 minutes of physical activity daily.
If you are just beginning, start with 10 minutes each day and gradually increase the duration.
Choose medium difficulty activities like brisk walking, jogging, swimming or dancing. Most importantly, choose activities and movements you enjoy- that way, you will be far more likely to commit to the regime.
Whilst there is nothing wrong with setting ambitious goals, break these down into small, achievable milestones. By doing so, you can maintain motivation.
Try cognitive behavioural therapy
Cognitive behavioural therapy seeks to alter a person’s behaviour by changing the way they think about events.
It is the gold standard of talking therapy and has proven efficacious in treating depression, anxiety and eating disorders, among other conditions.
It is not uncommon for those with obesity to suffer from mental health issues such as depression and anxiety.
What’s more, CBT can help obese individuals to challenge habits such as compulsive overeating by addressing ingrained but troublesome thinking patterns.
The human brain is remarkably adaptable, rewiring itself in response to experiences and repeated behaviours.
The brain’s ability to change its structure and function is known as neuroplasticity and explains why some behaviours become habits, such as putting on our seatbelt or scrolling on social media in the morning.
In short, each time you perform these behaviours, you reinforce neural pathways in the brain.
CBT seeks to challenge harmful habitual thinking patterns and substitute them with healthier ones. As it turns out, CBT may also be able to rewire the brain differently and build new neural pathways.
For example, obese individuals may lean on food as a comfort tool, leading to overeating and weight gain.
Often, this is a hangover from their upbringing, where food might have been associated with reward or affection.
During CBT, a therapist can help the patient challenge these thinking patterns and nurture a healthier relationship with food. They may also be able to rewire the brain and institute more sustainable eating habits.
Take special medications
Orlistat is the most common anti-obesity medication prescribed. The drug prevents around a third of the fat consumed from being absorbed in the gut. As a result, it leaves the body undigested in the stool.
Whilst these pills prevent further weight gain, they do not help reduce existing weight - this has to be done through healthier lifestyle habits and dietary changes.
Another weight-loss medicine prescribed to tackle obesity is Liraglutide. Taken as an injection daily, the medicine increases feelings of fullness, thereby preventing overeating.
Generally, these drugs are only prescribed if a person is unresponsive to other treatments after three months.
Use surgical methods of treatment
Suppose a person is severely obese, at high risk of developing complications and hasn’t responded to lifestyle, diet or pharmaceutical interventions. In that case, a doctor might suggest a surgical intervention in the form of a bariatric surgery.
In rare cases, surgery may be suggested as a first-line treatment, but only in people with a BMI over 50. There are three different types of bariatric surgery, namely:
Gastric bypass
A surgeon staples the top part of the stomach during this procedure, creating a small pouch that attaches to the small intestine. Food thus bypasses the larger stomach pouch, meaning you become full more quickly.
Gastric sleeve
A surgeon removes about 80 per cent of the stomach, creating a long, narrow pouch. The procedure is irreversible but can lead to significant weight loss.
Adjustable gastric band
A surgeon places a band around the top part of the stomach with an adjustable opening.
Over 160.000 bariatric surgeries are performed in the USA annually.
A gastric sleeve and bypass surgery increase the risk of vitamin and iron deficiencies. However, subsequent weight loss can positively affect potential obesity complications such as diabetes type II.
☝TOP TIP☝ Get genetic insights into your metabolism with the Atlas DNA Test.
Key points
- Obesity is a disease that increases the risks of other health conditions, including coronary heart disease, heart attack, diabetes, joint pathologies, oncology and hormonal disorders.
- Obesity is diagnosed by calculating the body mass index (BMI) or using other methods to determine the amount of fat in the body.
- The causes of obesity are plural and include diet, sedentary lifestyle, heredity, sleep patterns, emotional state, the presence of other diseases, and certain medications.
- The two primary interventions for obesity are increased physical activity and dietary changes
- The Atlas DNA Test can give important insights about metabolism and identify a genetic predisposition to obesity.
☝️DISCLAIMER☝This article is for informational purposes only. It is not intended to constitute or be a substitute for professional medical advice, diagnosis, or treatment.