We are trained to think that bacteria are bad rather than good, but gut microbes do far more for your health than antibacterial soap brands want you to know.
Yet the truth is not that straight-forward. The more we know about the symbiotic life of humans and bacteria, the more complex these relationships seem to be. Today, we’ll explain how bacteria do us a favour by protecting us from disease.
Bacteria are everywhere
Bacteria live all around you and on the surface of your skin, in your mouth, intestines, genitals and even in your eyes, which doctors previously thought to be sterile!
But don't freak out, bacteria have been there for ages (even millions of years, but don't take it personally), and most of them are not going to harm you. Quite the opposite. Since you are a team, bacteria are doing their best to make sure you live happily ever after.
Sure, some bacterial species may be harmful, but it usually happens when their numbers grow out of control or when the right bacteria for one place are accidentally transported to the wrong place. Here are some examples of this.
Staphylococcus aureus are common inhabitants of the nose and skin, but when they get into wounds or the bloodstream, they can cause infections that range from mild to serious.
Escherichia coli is an infamous culprit of food-related outbreaks, but that's only some members of Escherichia genus. It's actually normal to find low levels of these microbes in the gut. However, if they migrate to the urinary tract, they can cause an infection called cystitis.
☝️FACT☝️ Cystitis is more common in women because of the proximity between the urinary tract and the anus.
The problem with Petri dishes
Bacteria are hard to learn about and that's why it took so long for humans to figure out that all bacteria are not bad. In fact, many of them are vital for our wellbeing, and others, when in the right place at the right time, are unremarkable.
This revelation took a while to come about due to the fact that bacteria causing infections grew particularly well in Dr. Pasteur's Petri dishes. And many of the others, beneficial and commensal (usual and unremarkable), died when they were taken out of their comfort zone.
Some of them can't stand oxygen: these are called anaerobic. Others don't appreciate the light, and they live in places where the sun doesn't shine, like our intestines. #PunIntended.
☝️FACT☝️ Genetic sequencing of the gut microbiome allows researchers to identify novel microbes and assess their functions based on their DNA.
How does the microbiome protect us?
So there's still a lot for the scientific community to learn about microbes, possibly even centuries of new information to come. But they've already hit on a lot of interesting and important discoveries.
Bacteria protect themselves in their symbiotic communities and indirectly they also protect us using a variety of mechanisms. When they live in a happy, diverse and stable community, they complement each other by breaking down things into sources of sustenance for others.
They can also perform overlapping roles, so if one species is marginalised by an unexpected event (say a virus), others can take over performing that function. And these functions are imporant: producing vitamins and short-chain fatty acids (SCFAs) like butyrate, an anti-inflammatory compound that provides up to 90% of fuel for the gut lining.
In addition to that, bacteria, even the "good" ones, are able to defend themselves by making compounds that act as weapons to protect them against intruders. Some of them can even help prevent pathogenic species from sticking to the gut lining, thus inhibiting their ability to make us sick.
Gut microbes also digest much of our food that comes from plants because our body doesn't secret many enzymes that can take care of hard-to-digest dietary fibres. And in the process, the same way we digest food into poop, they digest our leftovers into nutrients that fuel and protect the gut, like butyrate.
The commensal bacteria in our colon have been training our immune system from birth to recognise them, and that is how they survive. At the same time, this work is what helps our immune cells recognise potential pathogens and mount a response.
Bacterial protection starts at birth
Some studies show that children born via C-section are more likely to develop metabolic and autoimmune diseases including diabetes type I, obesity, coeliac disease (serious gluten intolerance) and asthma.
Vaginally-born babies are exposed to immune-building microbes as they exit the mother's vaginal canal. But those born through C-section are not, and it has an impact on the development of their immune system and exposes them to long-term risks on their health.
It's called a bacterial baptism and it has some doctors very excited, and worried too. Because C-sections are becoming an increasingly popular delivery method around the world, even when it's not medically indicated.
That potentially means that less babies are being exposed to the protective film of microbes that builds their initial immune system. And this may increase the risk of infection and disease later on.
However, it's not all black-and-white because it never is in science: as we are reminded by the 2018 study, A Critical Review of the Bacterial Baptism Hypothesis and the Impact of Cesarean Delivery on the Infant Microbiome.
The authors indicate that, based on their review of current evidence, neonatal dysbiosis in C-section babies is likely to be influenced by a number of other factors including "post-partum antibiotic administration, absence of labor, differences in breastfeeding behaviors, maternal obesity, and gestational age".
That basically means that everything, from the choice of breastmilk and formula, whether the baby's birth was triggered by labour or induced with drugs, mother's weight, how many weeks the baby stayed in the womb (40 weeks on average) and the administration of antibiotics can all influence a child's budding immune system.
☝️DYSBIOSIS indicates negative alterations in the community of bacteria that compose a microbiome. In the case of newborns, it refers to unusual gut microbial patterns compared to babies born naturally. These changes may be linked to increased health risks throughout childhood and adulthood.
Microbiome patterns and chronic disease
There is a lot of time and finances being invested into research into the contribution of gut microbes to disease risk and protection. And it's money well-spent. In fact, there is already enough research for us to accurately assess your disease protection from 5 chronic diseases.
| METABOLIC DISEASES | Atherosclerosis |
| Diabetes type 2 | |
| Obesity | |
| INFLAMMATORY BOWEL DISEASE | Crohn's disease |
| Ulcerative colitis |
Identifying bacterial types that are present in the gut microbiome and their proportion in comparison to others and as a whole can reveal a lot of secrets about your health. While there is a lot to say on the subject, we can boil down the mechanisms so far elucidated to a few fundamental processes.
Diversity is a key trait for health, disease protection and the lack of it is an active trademark of certain disease patterns, like Crohn's disease. In atherosclerosis, a disease that causes narrowing of the arteries due to plaque build-up and often only detected when the patient has a heart attack, researchers note that gut microbial diversity is not affected but other parameters are.
Abundance of rare bacteria can be a problem. As stated above, we all have a few opportunistic beasties floating around in there, but that's okay because low amounts are normal. Yet, elevated representation of rare bacteria like certain types of E.coli or Proteus (typical in Crohn's and atherosclerosis respectively) indicate negative alterations to the ecosystem with adverse consequences.
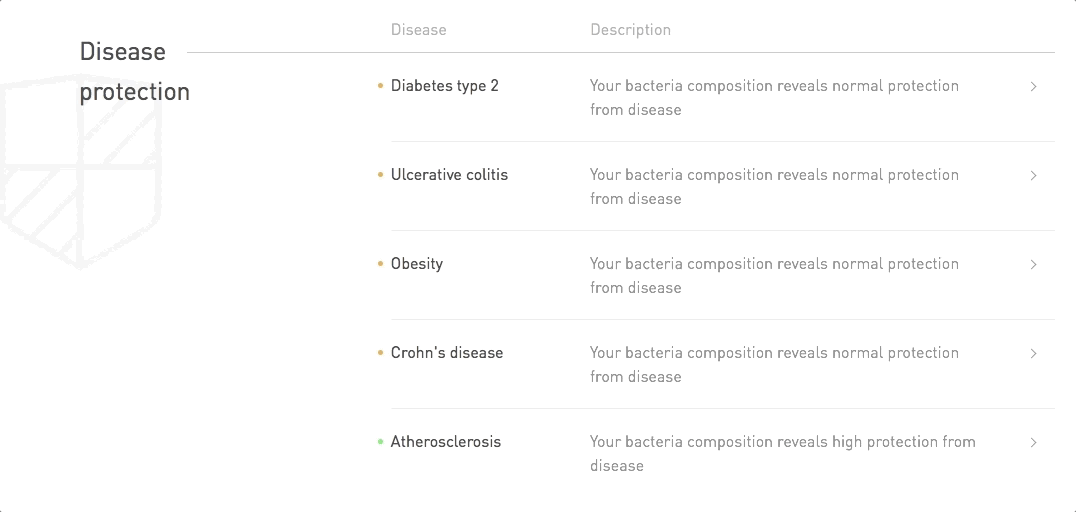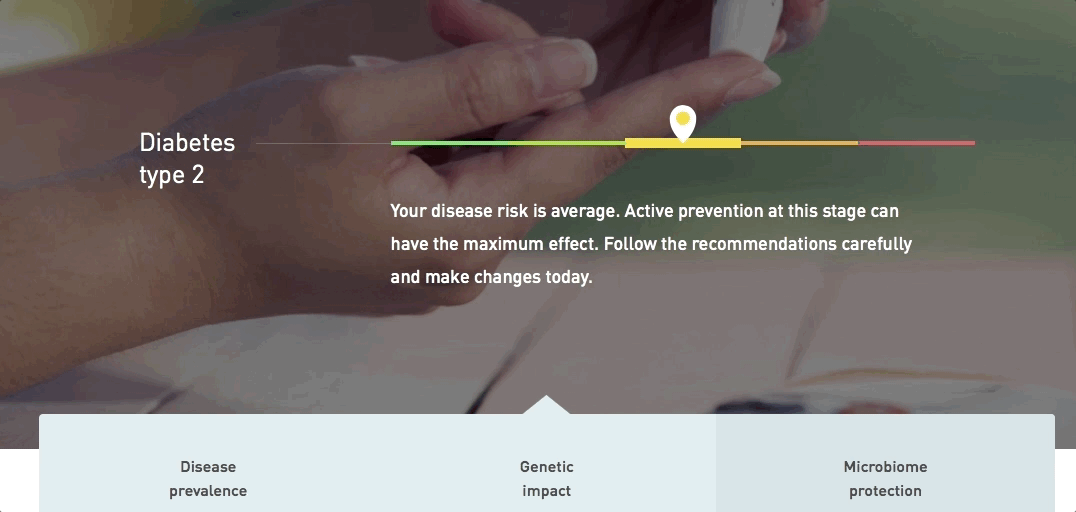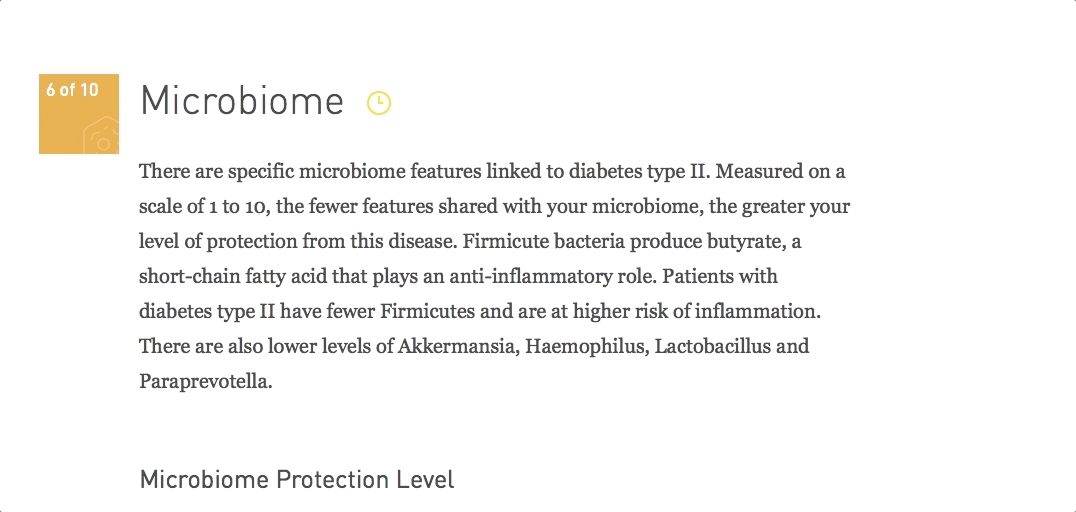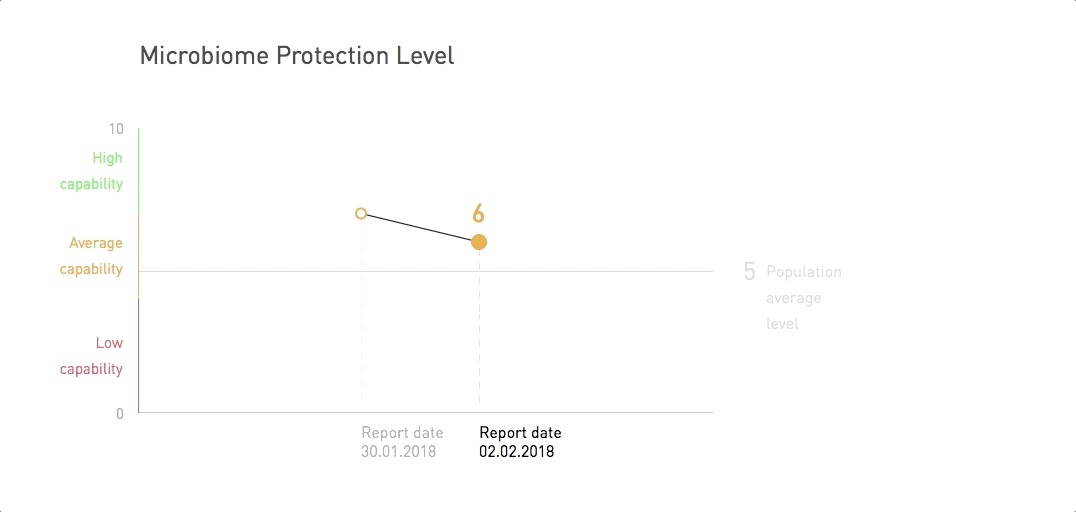
Lower levels of bacteria with anti-inflammatory properties is also a common marker in disease patterns. For example, Firmicutes, including Faecalibacterium prausnitzii are known for their butyrate-producing capabilities and may not be as abundant in the gut microbiomes of patients.
So the next time someone asks, you can tell them that gut microbial health is about far more than just farts, poop and the occasional dash to the privy after a bad curry.
☝️Remember:
1. Gut bacteria communicate and cooperate with the immune system.
2. A balanced ecosystem protects your body from certain diseases.
3. Dysbiosis is alterations in the ecosystem that can cause inflammation.
4. Vaginal birth "seeds" the newborn's microbiome that builds protection.
5. Gut microbiome testing helps assess disease protection.
- C Mueller and A J Macpherson. Layers of mutualism with commensal bacteria protect us from intestinal inflammation. Gut, 2006.
- Fabien Magne, Alexa Puchi Silva, Bielka Carvajal, and Martin Gotteland. The Elevated Rate of Cesarean Section and Its Contribution to Non-Communicable Chronic Diseases in Latin America: The Growing Involvement of the Microbiota. Frontiers in Pediatrics, 2017.
- LF Stinson et al, A Critical Review of the Bacterial Baptism Hypothesis and the Impact of Cesarean Delivery on the Infant Microbiome, 2018
- J. Zhuye et al., The gut microbiome in atherosclerotic cardiovascular disease, 2017
- C. Bogiatzi et al., Metabolic products of the intestinal microbiome and extremes of atherosclerosis, 2018
- NA. Molodecky et al. Environmental Risk Factors for Inflammatory Bowel Disease
- J E Mawdsley and D S Rampton, Psychological stress in IBD, 2005
- S. Khanna & LEH Raffals, The Microbiome in Crohn's Disease. Role in Pathogenesis and Role of Microbiome Replacement Therapies, 2017
- V. Pascal et al., A microbial signature for Crohn's disease, 2017