An in-depth look at what causes intolerance, how the microbiome can influence symptoms and the most common tests for lactose intolerance, including blood, breath, biopsy and stool tests.
Do you often feel nauseous, bloated or gassy after consuming dairy products? Love cheese but feel like you pay for every bite with abdominal pain and cramping? If so, you might be one of the many people worldwide who suffer from lactose intolerance.
Table of contents:
- What is lactose intolerance?
- Lactose intolerance tests
- The role of genetics in lactose intolerance
- The microbiome and lactose intolerance
- Takeaways
What is lactose intolerance?
Lactose intolerance is a common digestive issue where you cannot break down the sugar (lactose) found in milk. It happens when your small intestine does not produce enough lactase, the enzyme responsible for metabolising lactose. As a result, lactose passes through the small intestine into the colon.
When undigested lactose enters the large intestine, it is fermented by gut bacteria and converted into gases, including hydrogen and carbon dioxide. These byproducts cause the symptoms characteristic of lactose intolerance, including:
- abdominal pain
- bloating
- diarrhoea
- nausea
- flatulence
Both genetic predisposition and gastrointestinal issues can lower the production of lactase, leading to an intolerance.
Once upon a time, all humans were lactose intolerant in adulthood, losing the ability to produce lactase after infancy when milk was their primary food source. As humans began to domesticate cows and drink their milk products, certain populations experienced an advantage from sporadic genetic mutations.
In short, this beneficial mutation allowed them to produce lactase into adulthood, thereby giving them a new food source and increasing their caloric and nutrient intake.
☝Did you know?☝ Ötzi The Iceman, a 5300-year-old hunter-gatherer preserved in ice, was lactose intolerant.
For some, taking a lactase supplement when consuming dairy products can help, whilst others might find that probiotics alleviate symptoms (more on this later).
The human body cannot produce calcium from other nutrients, so it must be acquired through diet. If you are lactose intolerant, your doctor might suggest taking calcium and vitamin D supplements as both are essential nutrients needed for important bodily functions.
Lactose intolerance can be either permanent or temporary, depending on the underlying cause of lactose malabsorption and low lactase production. If these are triggered by undiagnosed coeliac disease, for example, treating this can eliminate lactose intolerance. This is known as secondary lactose intolerance. If poor lactase production is caused by genetic factors alone, it is known as primary lactose intolerance.
About 68% of the world’s population has lactose malabsorption, which means a reduced ability to digest lactose after infancy. Although related, malabsorption is not the same as an intolerance; all those with lactose intolerance have lactose malabsorption, but not all those with malabsorption have an intolerance.
There is a higher prevalence of lactose intolerance in those of Asian, African and Middle-Eastern descent, whilst it is far less common in Northern Europe, likely due to the fact that the climate historically allowed for daily cattle herding here.
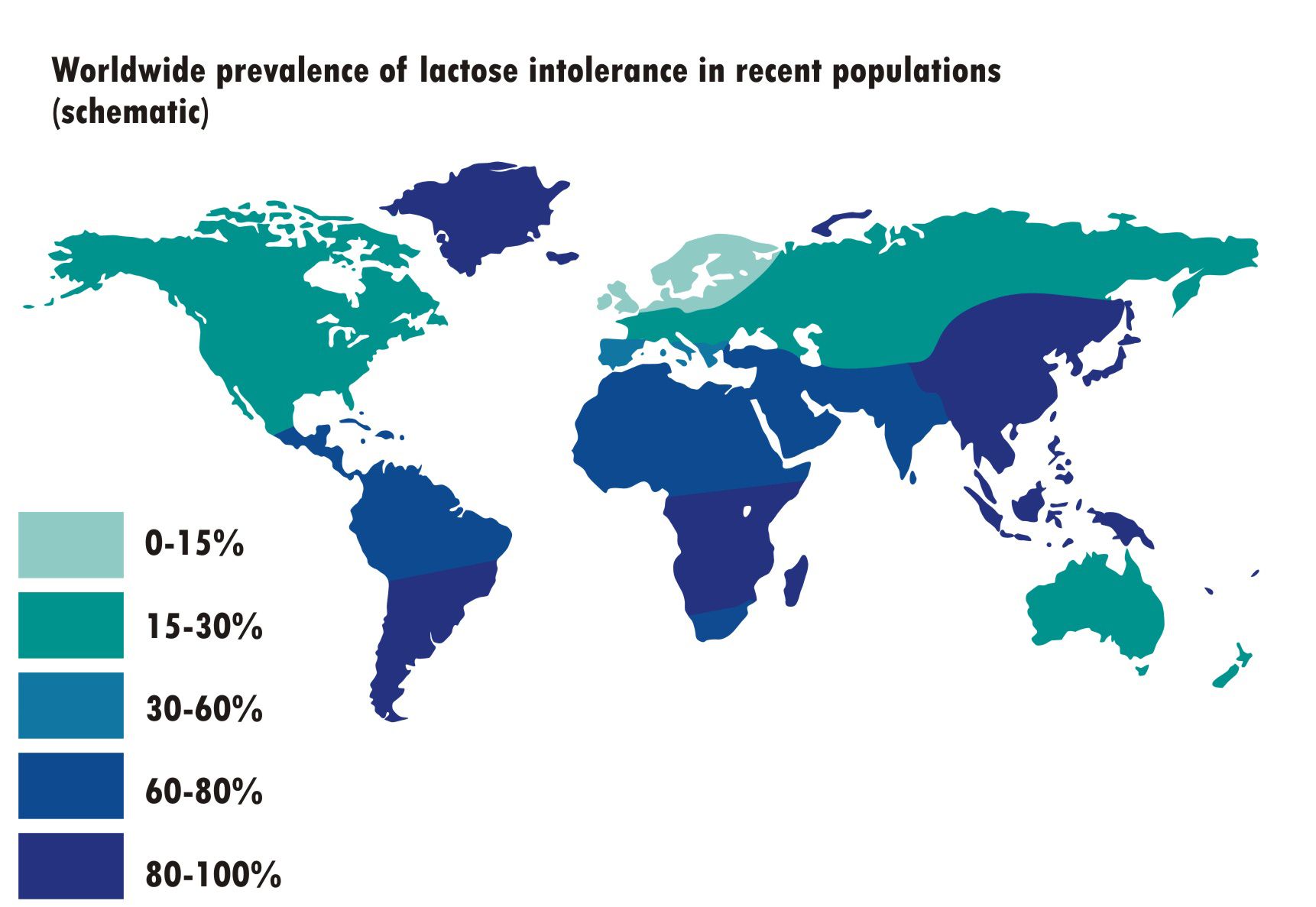
Lactose intolerance tests
The following tests can be used to either assist or reach a diagnosis of lactose intolerance. A physician might direct you to take more than one to establish a definitive diagnosis.
Hydrogen breath test
This is the most common test used by healthcare providers to diagnose lactose intolerance. It can be performed both at a doctor's office and at home. Shortly before the test, patients fast so that their baseline hydrogen levels can be measured. Antibiotics should not be taken in the two weeks prior to the examination.
To start, patients are given a drink high in lactose before having their breath measured at set intervals. On average, the test takes around 2 hours. The patient breathes into a bag that captures breath samples, allowing a doctor to measure the hydrogen levels as lactose passes through the digestive system.
When our bodies do not digest lactose it passes through to the large intestine, where bacteria break it down. This process produces various gases, including hydrogen. High levels of hydrogen indicate that your body is not producing enough lactase and that you might be lactose intolerant.
A short video demonstrating the hydrogen breath test.
Glucose blood test
In this test, glucose blood levels are measured before and after consuming a drink high in lactose. Like in a hydrogen test, the patient is asked to fast shortly prior to the examination.
When the body breaks down lactose normally, it is turned into glucose and galactose molecules. These are then absorbed through the small intestine and enter the bloodstream, raising the levels of both. If glucose levels do not become elevated after drinking a dairy product, it is an indication that insufficient lactase is being produced, a marker of lactose intolerance.
A concise clip demonstrating what a glucose blood test entails
Small intestinal biopsy
One of the rarer methods practitioners can use to detect lactose intolerance is a small bowel biopsy. This is where a sample of tissue is taken from the small intestine and tested to see how well the body produces lactase. Whilst invasive, the results from a biopsy can be more definitive than other methods.
A small intestinal biopsy can be painlessly performed during a routine endoscopy, though it is rarely the method of choice when testing for intolerance. This is largely because it is an invasive procedure. A physician might opt for a biopsy to rule out secondary intolerance caused by things such as coeliac disease.
Stool Acidity Test
Stool acidity tests are used to diagnose intolerance in infants and younger children. In this test, a doctor gives the patient a drink high in lactose and then examines their stool sample.
In those with a normal tolerance to lactose, the drink will be absorbed without problem in the small intestine. Whilst variable, healthy stool is usually alkaline. For those with an intolerance, the lactose will pass undigested to the colon where bacteria begin fermenting it and produce acid; as such, high acidity levels in the stool indicate lactose intolerance.
The role of genetics in lactose intolerance
In the Atlas DNA Test, we analyse your genes and look for two variants of the MCM6 gene; this controls the activity of the LCT gene, which encodes the lactase enzyme. By doing so, we can determine if you are genetically predisposed to lactose intolerance.
This can assist in the diagnosis of primary lactose intolerance, but it cannot determine whether you are lactose intolerant alone. If you are predisposed to lactose intolerance, you should seek further testing.
The microbiome and lactose intolerance
Lactose intolerance is primarily a genetic trait, but recent studies show gut bacteria can influence how well the body tolerates dairy products. This is because certain microbes can break down and absorb lactose without producing much gas, even in those who suffer from lactose intolerance. These include:
| Lactobacillus | Bifidobacterium |
| Faecalibacterium | Roseburia |
In the Atlas Microbiome Test, we look at the proportions of these beneficial microbes in your stool; the fewer of these lactase-producing bacteria that are present, the lower your lactose metabolism score will be. If you do not suffer from lactose intolerance, then limited microbiome lactose digestion will have no effect.
In those with lactose intolerance, a lack of beneficial bacteria could exacerbate symptoms. On the upside, cultivating bacteria like lactobacillus and bifidobacterium could soothe them.
Interestingly, studies have found that galactooligosaccharides (GOS) supplements can reduce the side effects of lactose intolerance, namely cramping, stomach pain and diarrhoea. This is because GOS are prebiotic molecules that feed beneficial bacteria.
☝TIP☝ If you have trouble digesting dairy products, head to your personal account and find out what your Atlas Microbiome Test says about your bacteria and lactose metabolism.
The takeaway
- Lactose intolerance is more prevalent in those of African, Middle-Eastern and Asian descent
- Lactose intolerance occurs when the body does not produce enough lactase, meaning the small intestine cannot breakdown and absorb lactose
- It is estimated that 68% of the world's population suffer from lactose malabsorption
- Hydrogen breath tests are the most common medical testing method, whilst a small bowel biopsy is the least common
- A DNA test can reveal whether you are predisposed to lactose intolerance
- Specific probiotic bacteria can alleviate the symptoms of mild-moderate lactose intolerance
☝️DISCLAIMER☝This article is for informational purposes only. It is not intended to constitute or be a substitute for professional medical advice, diagnosis, or treatment.
















