Here’s what you need to know to restore gut health, help your natural flora, and choose the gut health supplements after antibiotics.
Becoming your healthiest self can feel like an insurmountable task, especially because our bodies can be wildly mysterious and complex. But many people don’t know that there are simple, specific, studied ways to improve your health – and most of them have to do with the gut.
This is because your body relies on good bacteria to regulate the digestive system, support immunity, serotonin production and much more. Rather than figuring out how to get rid of bad gut bacteria, you’ll discover that restoring gut flora and fixing good bacteria is more important.
Table of contents
- What is the gut microbiome?
- Good bacteria for gut health
- Gut bacteria and immune health
- How do antibiotics damage your gut health?
- Common antibiotic side effects
- The best ways to restore gut health
- How long to repopulate good gut bacteria?
- How to restore healthy gut flora
- Probiotics for antibiotic side effects
- The long-term effects of damaged gut health
This article is by our friends over at Jetson Probiotics. Keep reading to discover how probiotics can mitigate the effects of antibiotics alongside other ways to take care of your intestinal microbiome.
☝️DISCLAIMER☝This article is for informational purposes only. It is not intended to constitute or be a substitute for professional medical advice, diagnosis, or treatment.
What is the gut microbiome?
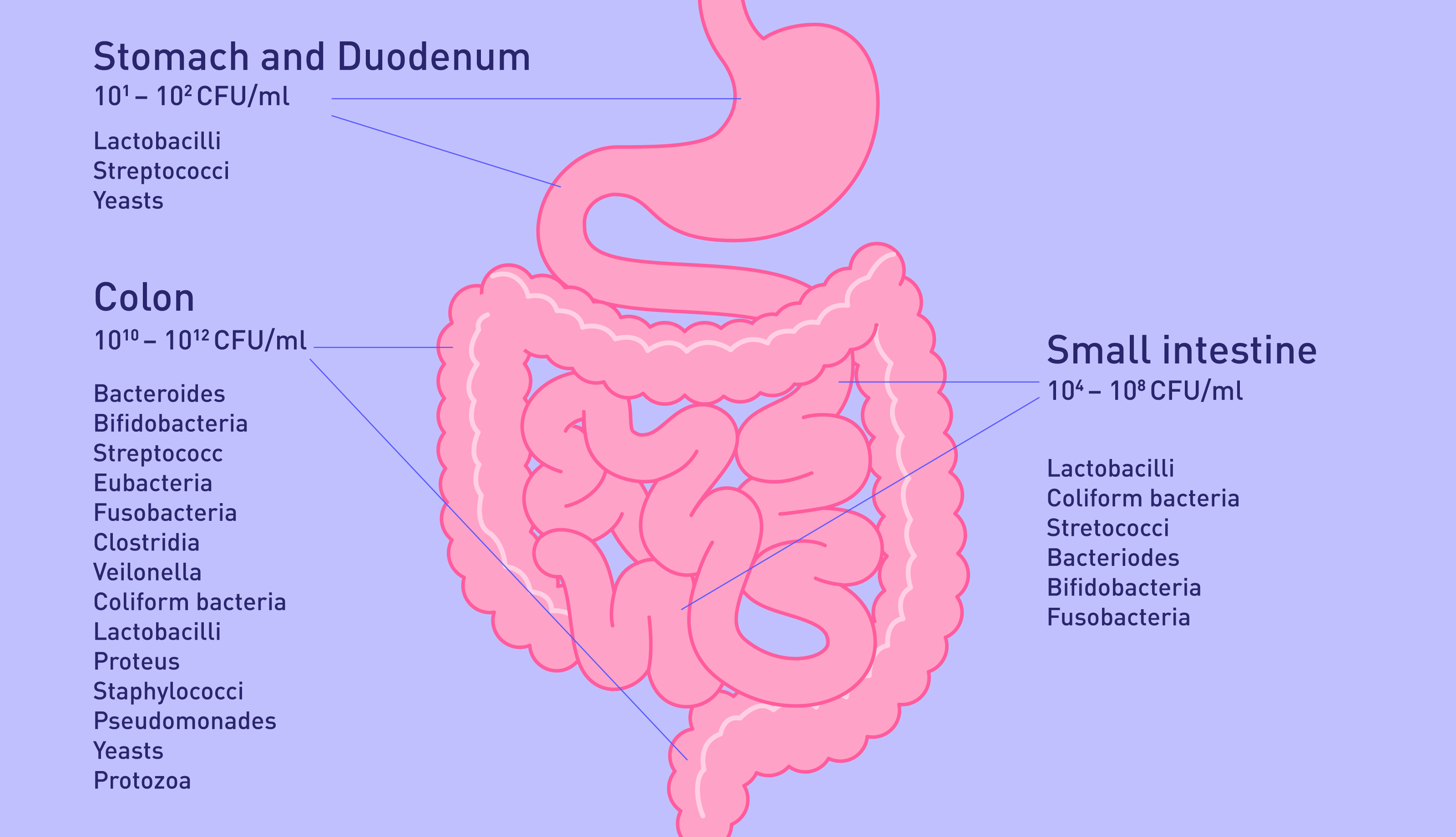
Your gut microbiome lives in your large intestine, and it’s home to the most diverse bacteria in your entire body. That’s because, unlike any other part of the body, your digestive tract is an open ecosystem, which is more exposed to its external environment than any other part of the body.
What does this mean? Well, the gut microbiome can be shaped by things like gender, age, geographic and socio-economic conditions, diet, and health conditions. It also means that every person’s gut microbiome will be different, and affected by different factors.
Good bacteria and gut health
But we’ve been told for decades that all bacteria are evil, so if you’re wondering, “Is flora good for you?” right now, then you’re not alone. Don’t worry, this widespread belief is a myth. In fact, now we know that bacteria are overwhelmingly harmless, some are great, and only a few are bad.
For your gut to stay happy and keep you healthy, it depends on microbial diversity. Basically, there must be lots of different types of microbes living together. When there isn’t, it leads to dysbiosis, in which there isn’t enough diversity and some bacteria can grow out of control.
When an imbalance of good and bad bacteria happens, the microbiome can become unhappy, and this has consequences for digestion, inflammation, the gut lining, and even mood and brain health.
☝Say hello to your little friends!☝ Discover the diversity and composition of your gut bugs with the Atlas Microbiome Test.
Gut bacteria and immune health

Most importantly, a takeover of bad bacteria can dramatically affect immunity and leave room for infection, disease and chronic illnesses to develop. The gut is the first line of communication between the external environment and the immune system. The two work together to mutually regulate our body’s reaction to harmful pathogens.
But when the immune system and gut are working together, things are working smoothly. This encourages the growth of beneficial bacteria, which improves immunity and gut function. It creates stronger responses to pathogens while makes the body more tolerant to your natural gut bacteria.
How do antibiotics damage your gut health?
Antibiotics are prescribed to nearly half the UK population every year for common conditions and in hospitals to treat and prevent serious infections. Here are the most common applications for antibiotics:
| ear infections | sinus infections |
| chest infections | throat infections |
| urinary tract, bladder and kidney infections | skin and wound infections |
| pneumonia |
Unfortunately, antibiotics don’t stop at bad bacteria and they don’t treat viral infections, which are often nearly impossible to distinguish from bacterial ones. Instead, antibiotics kill good bacteria too, and that’s bad because good bacteria are often helping your body fight the infection.
Many people also experience mild-to-severe antibiotic side effects, especially if their immune health is already compromised, like hospital patients. More seriously, antibiotics can leave room for extremely harmful bacteria such as E.coli, C.diff and Salmonella – infections that may be so severe that hospitalization is required.
Common antibiotic side effects
- diarrhea
- yeast infections
- gas
- vomiting
- nausea
- constipation
Even though antibiotics are very effective at clearing up bacterial infections, it’s important to take the necessary precautions to bolster your gut microbiome, because keeping the good bacteria is just as important as killing the bad.
What are the best ways to restore gut health?

It’s no secret that gut health is a non-negotiable to achieving overall health. Maintaining levels of good bacteria in the gut microbiome can be done through a number of ways, including diet and the use of probiotics.
It starts with your diet. Good bacteria feast on fibers and nutrients in plant foods – these are prebiotics – and they turn these substances into nutrients that nourish your gut lining and keep your gut biome balanced.
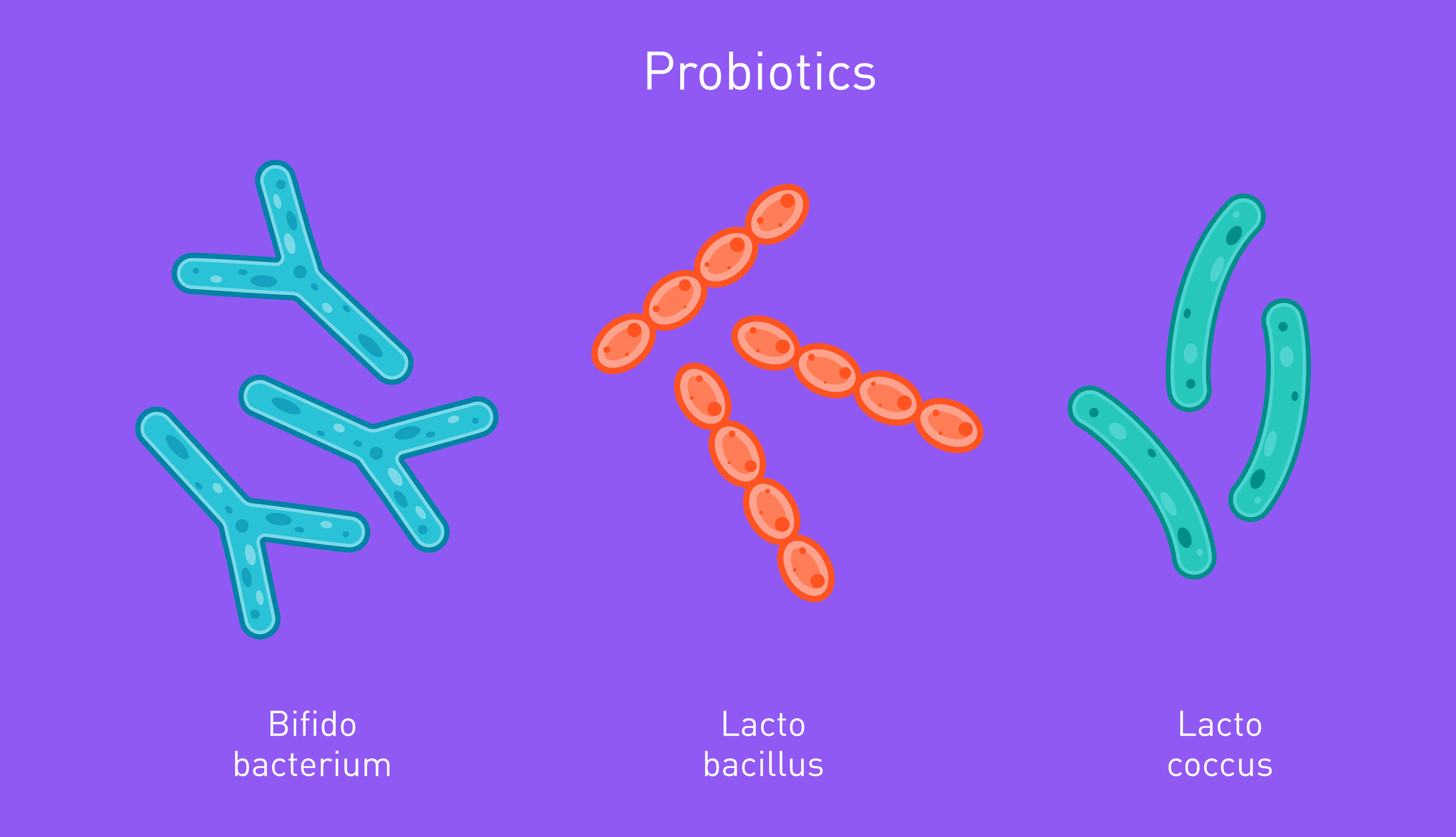
Alternatively, probiotic supplements contain billions of bacteria from one or several bacteria strains that in specific, studied doses have benefits for your health. Here are some of the most famous and well-researched probiotic bacteria and yeasts that you will find in supplements:
| Bifidobacterium | Lactobacillus |
| Lactococcus | Saccharomyces |
☝️What Atlas Biomed says:☝️ the microbiome scientists at Atlas highlight that the benefits of probiotics may be temporary for some people, and only last as long as they are taking supplements.
How long does it take to repopulate the gut with good bacteria?
There’s no simple answer to this question because it depends on the state of your microbiome, the quality of your diet, any medication you take, your level of exercise and more. However, the gut microbiome is very adaptable and responds to positive lifestyle choices.
So if you eat a diet with lots of fiber-rich whole foods (something scientists like to call prebiotics) and add some probiotic foods or supplements, you can speed up your gut biome restoration. Plus, getting regular exercise, especially cardio, is associated with higher diversity in your gut.
How to restore healthy gut flora
Probiotics are generally safe, and sometimes even recommended to take during a course of antibiotics, except for hospitalised patients and people with compromised immune systems. They are especially helpful afterward to support the recovery of your gut microbiome.
☝️TIP☝️ There is no such thing as a clean gut diet – your gut naturally cleans itself. However, you can help your gut bacteria keep you healthy with a plant-rich prebiotic diet.
What probiotics for antibiotic side effects?
Typically, it will take the body time to balance the microbiome to healthy, diverse bacteria levels. In fact, research shows that it takes about 6 months to recover from the damage done by antibiotics. And even then, the body might not even be back to its pre-antibiotic state.
Saccharomyces boulardii, a probiotic yeast is particularly good at preventing and alleviating antibiotic-associated diarrhea and traveller’s diarrhea. It’s also a friend to your gut bacteria that supports good bacteria and prevents inflammation.
Lactobacillus acidophilus, a probiotic bacterium best known for being in yoghurt is also great for your gut. Studies show that it’s good at treating and preventing infections, and reducing the digestive side effects of antibiotics.
Other bacteria that help recover from antibiotic use include:
- L. casei
- L. Rhamnosus GG
- L. Plantarum 299v
- B. subtilis
- B. coagulans lactospore
- B. clausii
What are the long-term effects of damaged gut health?
Not only is your body more susceptible to infection, weakened immunity, and chronic inflammation, but we also know that an imbalanced microbiota can increase risk for later-onset of chronic disease like heart disease, diabetes, even Alzheimer’s Disease and Parkinson’s.
The gut microbiome is the most bacterially diverse part of your body, and it’s impacted by what you eat, drink, your activity levels, and the medications you take. It may seem a bit overwhelming, but it doesn’t take much to fix your gut: good food, regular exercise, and some help from probiotic bacteria.



















